Collected data
Available data in FaMe-Net

Data from each encounter
The care providers of the participating general practices register all encounters with their patients using the International Classification of Primary Care (ICPC-2). All encounters are registered in episodes of care, which is explained on the homepage.
For each encounter, the following variables are systematically coded:
- Reason for Encounter (RFE)
- Diagnosis
- Diagnostic and therapeutic interventions
- Measurements
- Medication
Patients can have contact with their general practice in different ways: physical consultation, telephone consultation, home visit or e-consultation.
Data from specialists and other healthcare providers
GPs receive letters from other healthcare providers in primary and in secondary care concerning a patient’s health problem. These letters are added to the patient’s Electronic Medical Record and are assigned to an episode of care.
The information in the letter may result in modifying the diagnosis of the episode of care. A letter may also contain information on a health problem that was not yet known by the GP. In that case, it results in the start of a new episode of care.
Data from after-hours GP care
During after office-hours, general practice emergency care is provided by a GP medical post. All encounters (physical consultation, telephone consultation, home visit) with this medical post are included in the patient’s electronic medical record. The FaMe-Net GPs add the codes of the RFE, diagnosis, performed interventions, measurements and medication for the out-of-hours encounters.
Personal and contextual characteristics of the patient
FaMe-Net has started to collect contextual and personal characteristics of all the enlisted adult patients in a structured way since 2016. Upon invitation by email, patients complete a questionnaire about personal and contextual characteristics, including for example level of education, country of birth of patient and parents, intoxications, psychotraumatic life events, and information on the family history for diabetes, cardiovascular disease and several cancer types.
Patients are invited to update the context survey periodically.
FaMe-Net derives the socio-economic status (SES) from the highest completed educational level, in accordance with Statistics Netherlands’ advice
Systematically coded variable data explained
All presented symptoms, complaints, and diseases are classified in accordance with the International Classification of Primary Care (ICPC-2) at the highest level of accuracy and understanding. In addition to ICPC-2, diagnoses are also coded with the International Classification of Diseases and Related Health Problems (ICD-10).
Transfer to ICPC version 3 is planned, now that it has been released in December 2020. This will allow for additional recording of functioning (activities and participation) and personal preferences linked to morbidity.
In FaMe-Net, all morbidity is registered in episodes of care. An episode of care can be defined as ‘a health problem presented by an individual to a healthcare provider, from the first presentation until the last encounter’. The title of an episode of care is the episode diagnosis, classified with ICPC-2. The episode diagnosis can be modified during the episode of care. For example: an episode of care is first labelled as fatigue, but after laboratory testing, the diagnosis (episode title) is changed to iron deficiency anaemia, and it later appears to be caused by colon cancer, which will be the final diagnostic label. All contact elements related to this health problem are comprised in this episode of care, including specialist reports to the GP. We often abbreviate ‘episode of care to ‘episode’.
In our infographic, we explain how the Episode of Care is built from one or multiple contacts between patient and general practitioner (GP).
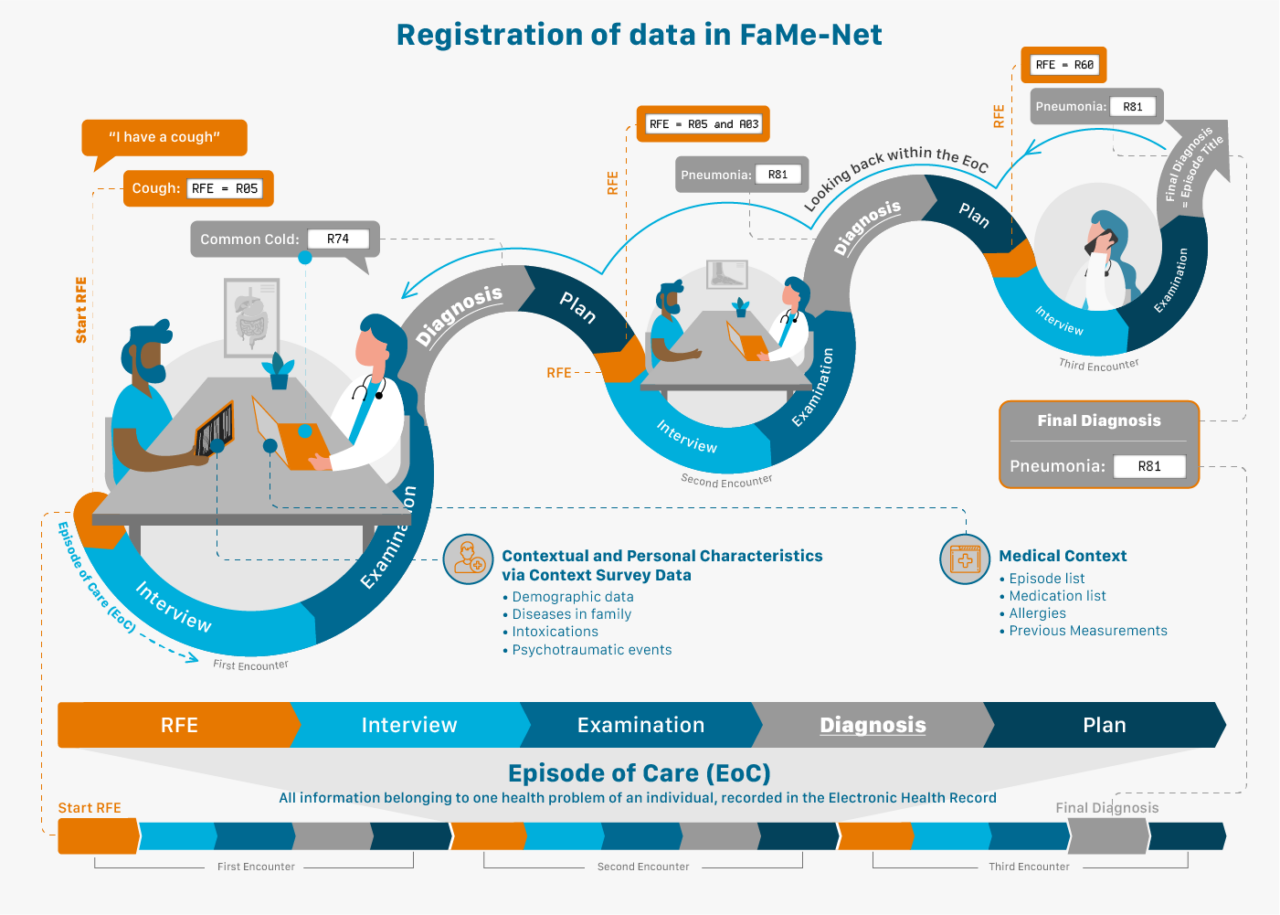
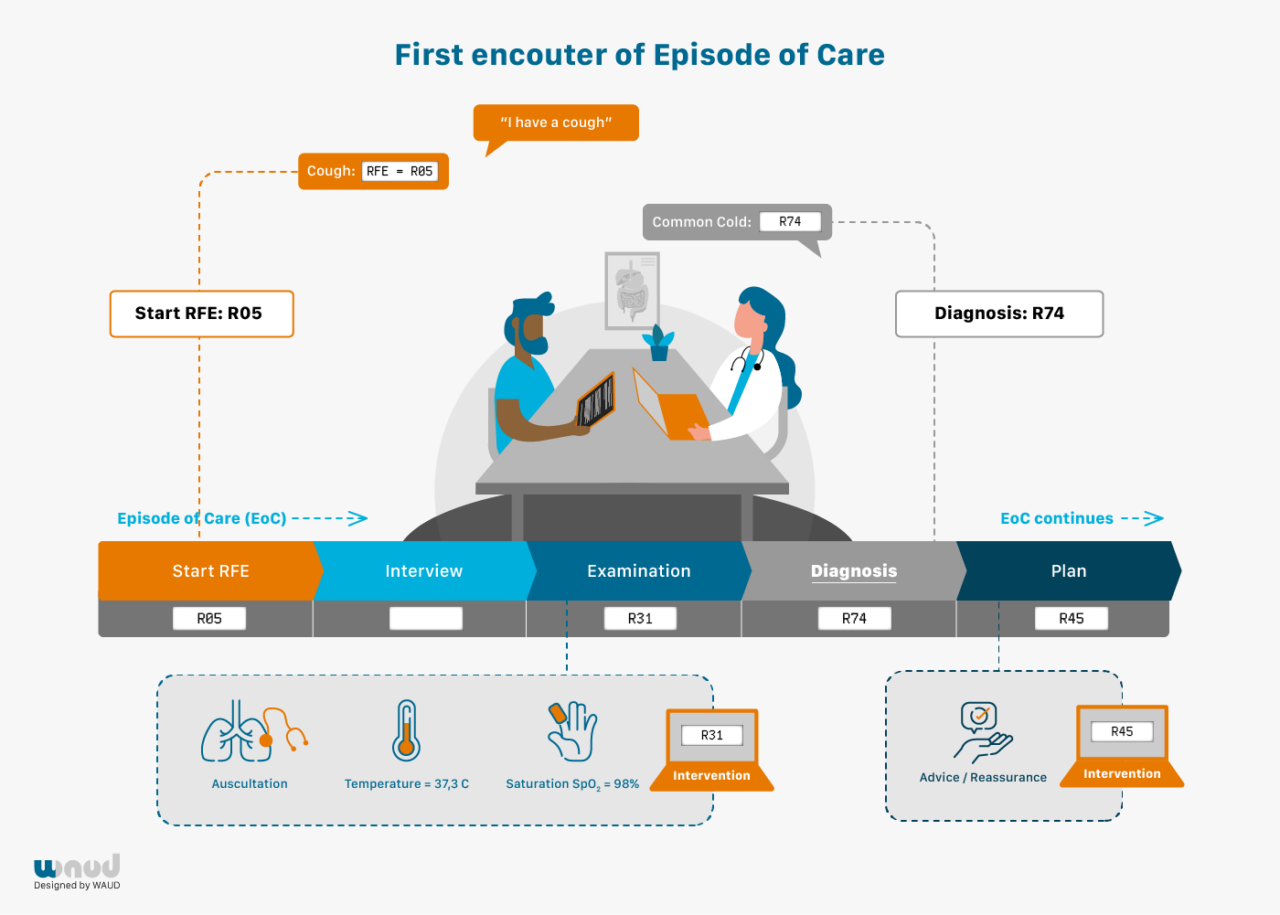
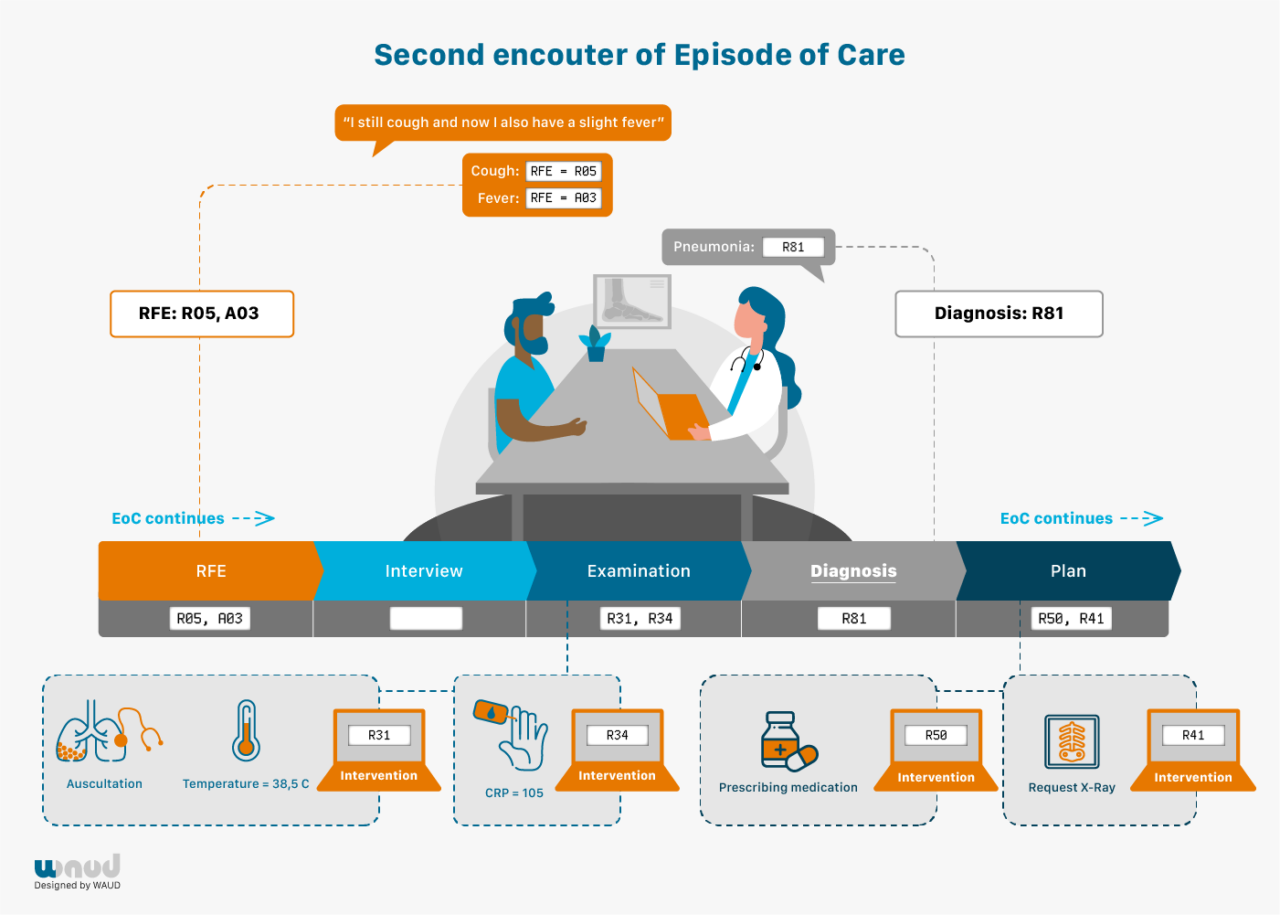
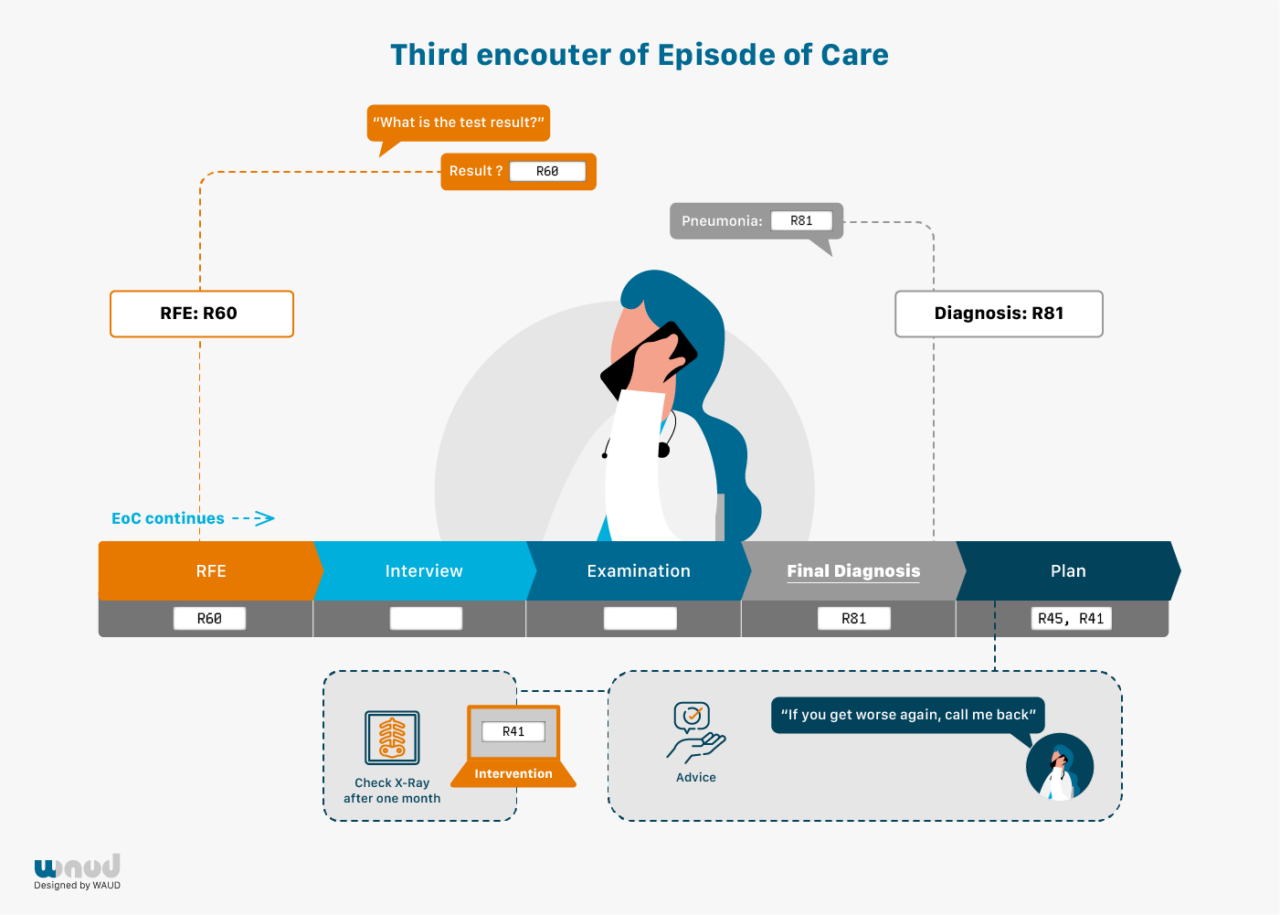
Every encounter starts with coding the Reason for Encounter (RFE). This is the spontaneous statement of the patient on why they visit the care provider. This reflects the initial presentation of the illness. This statement precedes the interaction between patient and GP and precedes the GP’s interpretation. FaMe-Net routinely and systematically registers all RFEs in all encounters.
The RFE(s) can be presented as a symptom (e.g. abdominal pain, a rash, cough), but also as a self-diagnosed or suspected disease (‘I’ve got the flu’; ‘I think I have migraine’; ‘I hope it’s not pneumonia again’) or a request for a particular intervention (‘I would like to have a blood test’). When multiple RFEs are presented, all are registered. The RFE(s) should be recognised by the patient as an acceptable description of the demand for care. RFE registration enables research studying associations between RFE and (final) diagnosis. RFEs have important prognostic value, for example in diagnosing cancer. RFEs are coded according to the ICPC-2.
Since 2016, the duration of the RFE (the duration between the start of the complaint and the GP encounter) is also coded in every encounter.
Diagnoses are coded according to the International Classification of Primary Care (ICPC-2) at the highest level of accuracy and understanding. This means that diagnoses are coded as a symptom (e.g. fever of back complaints) when no disease can be diagnosed and are coded as a disease (e.g. infection or back syndrome) when the care provider is convinced of a disease as diagnosis. In addition to ICPC-2, diagnoses are also coded with the International Classification of Diseases and Related Health Problems (ICD-10). The episode diagnosis can be modified during the episode of care.
All diagnostic and therapeutic interventions are coded according to the ICPC-2. Examples of interventions are diagnostic imaging, laboratory testing, medication prescription, health advice, surgical procedure, and referral to primary or secondary care professionals.
The intervention ‘medication prescription’ is followed by the type of medication that is prescribed.
The intervention ‘referral’ and ‘consultation’ is followed by the specialism that is referred to (e.g. neurology of physical therapy).
All measurements made during an encounter are systematically registrated in the electronic medical record. This concerns measurements in the physical examination (e.g. temperature, blood pressure, oxygenation), variables resulting from the patient interview (e.g. smoking status) and results from laboratory testing.
All medication prescriptions are coded according to the Anatomical Therapeutic Chemical (ATC) coding system maintained by the World Health Organization.
Click here to visit the ATC-Classification website.
